Yeast Infections: Certain Women are at Greater Risk

Learn why some women are more likely than others to contract yeast infections. Yeast infections, also known as candidiasis, are infections caused by a yeast (a type of fungus) called Candida. Yeast infections are more common than you might think. About 75 percent of women have had a yeast infection, and about 45 percent will have them more than once. About 1.4 million outpatients of candidiasis are seen annually in the United States. Why do Women Get Yeast Infections? All healthy vaginas have yeast. Candidiasis is caused by an overgrowth of yeast that causes infection. Any woman at any age can get a yeast infection, although it is rare before puberty and after menopause. Learn more about yeast infections here, including symptoms, diagnosis and treatment. In this blog, we’re going to dive deeper into why some women are at greater risk. Who is at Risk of a Yeast Infection? Some women are at greater risk of getting a yeast infection. Here are some risk factors. Pregnancy: If you are pregnant or on birth control, the risk is heightened because estrogen is a factor in maturing the vagina and making a thicker lubricated vaginal lining. Damp places increase the growth of yeast, and estrogen is increased with birth control and pregnancy. Diabetes: Diabetes increases the risk of yeast infection because it is caused by excess glucose in the blood. Because of this excess glucose, more is secreted from the vagina, which is normally an acidic environment that has little nutrients. This glucose promotes the growth of yeast. Immune System Deficiencies/Antibiotics/Steroids: Women with weakened immune systems are at greater risk for developing yeast infections because their bodies aren’t capable of defending themselves from infections. Additionally, immune system problems are often treated with antibiotics or steroids, which increase the risk of yeast infections because antibiotics kill off the bacteria that maintain and limit the growth of yeast. Without that bacteria to do its job, yeast has an ideal environment to grow rapidly and turn into an infection. Sex: Sexual interactions are not the cause of yeast infections, but yeast can be spread vaginally and orally. The chemistry of the different yeasts may be different and unbalanced, which can cause it to grow. Yeast infections aren’t an STD, but a person’s body chemistry can have a bad reaction to another person’s yeast and bacteria. How to Prevent Yeast Infections It’s important to know who is most at risk for yeast infections, and it’s also smart to learn prevention. Here are a few key preventions: Watch antibiotic use. Only take antibiotics when prescribed by a doctor. Wear cotton underwear. The cotton allows airflow, which prevents the vagina from getting too damp. (Yeast prefer damp environments.) Don’t douche or use scented feminine products. These products can kill the healthy bacteria that limits yeast growth. Wipe from front to back after using the restroom. Avoid moist environments, such as tight, wet clothes, hot tubs or hot baths. Conclusion: Yeast Infections are Common Yeast infections are common occurrences among women of all walks of life. Luckily, there are ways for women to lower their risk of contracting a yeast infection. If you think you have a yeast infection, there are many treatment options. Make an appointment with your physician to ensure you receive the correct care and advice.
What Women Need to Know About Osteoporosis

Osteoporosis is a bone disease that occurs when the body cannot replenish its bone tissue as quickly as it wears away. And it’s common in post-menopausal women. “I was a very nervous kid, I was anxious all the time when I was younger, but what’s nice is that some of the things I was anxious about don’t bother me at all anymore. Like, uh, I always thought that quicksand was going to be a much bigger problem than it turned out to be…I used to sit around and think about what to do about quicksand. I never thought about how to handle real problems in adult life, I was never like, ‘Oh, what’s it gonna be like when relatives ask to borrow money?’ “ -John Mulaney, New In Town As a child, most of us never worried if we were getting enough calcium in our diets. Like John Mulaney, we were worried about quicksand and anvils falling from the sky. But as we get older, what we worry about changes, and as middle age approaches, osteoporosis and calcium-deficient diets become even greater worries. The human body uses calcium for a number of tasks: calcium regulates nerve signals, including those used to release hormones such as insulin. Calcium in the bloodstream also regulates how muscles and blood vessels contract and dilate, and it continues to do this for the duration of a person’s life. If the available calcium begins to diminish, the body will pull calcium from the stores in the bone tissue. This deficiency is the beginning to the disease known as osteoporosis. Osteoporosis is directly responsible for 1.5 million fractures every year. Ten million Americans are affected by this affliction today. Women are four times more likely than men to develop this disease, and half of all American women will break a bone due to osteoporosis after the age of 50. After menopause, a woman’s risk of breaking a hip is equal to her combined risks of breast, uterine and ovarian cancer. Why Does Osteoporosis Affect Women? Osteoporosis affects post-menopausal women in greater quantities than any other group of people. This bone disease that occurs when the body cannot replenish its bone tissue as quickly as it wears away. The body stores nearly all of its calcium in bones, and pulls calcium from the bone tissue as it needs. As a result of the body slowing down its bone production, the patient may lose too much bone mass or makes too little new bone tissue — or both. As a result, bones become porous as they become increasingly calcium deficient. They quickly become weaker and may break easily — in severe cases, bones can break from a sneeze. Aging in men and women slow down their endocrine systems, which affect bone production. However, the cessation of estrogen manufacturing in women is significantly more dramatic than the slowdown of men and their hormones. Additionally, women have smaller bones than their male counterparts, which means smaller stores of calcium, all resulting in an increased risk for osteoporosis. How Can Women Combat Osteoporosis? There are a number of things a woman can do, or stop doing, to strengthen her bone tissue and stave off osteoporosis. Women over age 50 should take between 1,200 and 2,000 milligrams of calcium daily. One of the best ways to prevent osteoporosis is to ensure a plentiful amount of calcium is available for the body. It is especially important to supplement your diet with calcium if you happen to be: Vegan Following a high protein diet Following a high sodium diet Suffering from Crohn’s disease, IBS or another health condition that limits your body’s ability to absorb calcium Under treatment with corticosteroids for an extended period of time Who is at Risk for Osteoporosis? Other factors that raise the risk of osteoporosis include: Cigarette smoking Excessive alcohol and/or caffeine consumption Lack of exercise A diet low in calcium Malabsorption (nutrients are not properly absorbed from the gastrointestinal system) from conditions such as Celiac Sprue Chronic diseases such as rheumatoid arthritis and chronic hepatitis C, an infection of the liver Immobility, such as after a stroke, or from any condition that interferes with walking Vitamin D deficiency. Vitamin D helps the body absorb calcium. When vitamin D is lacking, the body cannot absorb adequate amounts of calcium to prevent osteoporosis. Vitamin D deficiency can result from lack of intestinal absorption of the vitamin such as occurs in celiac sprue and primary biliary cirrhosis. Certain medications can cause osteoporosis. These include heparin (a blood thinner), anti-seizure medications phenytoin (Dilantin) and phenobarbital, and long term use of corticosteroids (such as Prednisone). Calcium supplements can have a positive affect, even if a patient is already suffering from osteoporosis. Also, a balanced diet with adequate calcium and vitamin D assists in staving off the disease — as do medications that stop bone loss and increase bone strength, such as risedronate (Actonel), and calcitonin (Calcimar). How Do I Know if I Have Osteoporosis? If you or someone you know has reached menopause, then you should get a bone density test to determine the risk of having this disease. You can contact us to set up a time to determine your risk of osteoporosis. A Bone Mineral Density (BMD) test uses a pair of low dose X-rays to measure density and thickness of the bones in the hip and spine. You cannot see or feel your bones becoming thinner or weaker. Bone Mineral Density (BMD) testing is used by health care providers to diagnose osteoporosis. The BMD test determines bone density by assessing the quantity of minerals (calcium and phosphorus that your bone contains. A dual X-ray absorptiometry (DXA) of the hip and spine is a quick, painless, low-dose X-ray that measures the density or thickness of your bones. BMD testing provides a T-score that compares your bone density to the average bone density of young healthy adults of the same gender. A T-score above -1.0 typically represents normal bone mass. Low bone
Ovarian Cysts: What Are They, and How Are They Treated?

Ovarian cysts often go away on their own. Here’s what you need to know about this common women’s health condition. September is Ovarian Cancer Awareness Month, and we at Women’s Integrated Health can’t stress enough the importance of regular health screenings, including yearly women’s wellness exams, to aid in early detection of issues that could risk a woman’s health. Because attention is on ovarian cancer this month (and hopefully always), let’s talk about ovarian cysts, which can occasionally be cancerous. Doctors can detect ovarian cysts during regular pelvic exams by feeling for swelling on the ovaries. If a doctor suspects a cyst, he or she will perform an ultrasound to confirm the diagnosis. What is an Ovarian Cyst? Ovarian cysts are solid or fluid-filled sacs or pockets within or on the surface of an ovary. They’re surprisingly very common. Doctors see more than 3 million cases yearly in the United States. Most ovarian cysts are symptom free and disappear on their own within a few months. Occasionally, ovarian cysts linger, causing complications: Signs of Ovarian Cysts Menstrual irregularities Pain during intercorse Irregular bowel movements If ovarian cysts cause issues, there are a few medical treatment options doctors discuss with their patients. [highlightbox color=”alert-success”] In the News: Pop star Kelly Clarkson talks about her painful experience with ovarian cysts. [/highlightbox] Medical Treatments for Ovarian Cysts Hormonal birth control pills. Birth control pills can regulate a woman’s hormones to get cysts in check. Plus, they reduce the risk of developing more cysts. Surgically removing the cyst. For this surgery, a doctor creates a small incision in the navel or stomach to remove the cyst. Removing the ovary or fallopian tube. In rare cases, a cyst can damage the ovaries or fallopian tubes. In these instances, one or both of these organs could need to be removed. Can Ovarian Cysts be Cancerous? It’s important to note that only about 5-10 percent of women with ovarian cysts require surgery. And of those women, only about 12 percent are cancerous. If a doctor finds an ovarian cyst, he or she will most likely order imaging tests and/or biopsies to determine whether the cyst is cancerous. In the event a cyst is cancerous, treatments include chemotherapy, radiation and surgery. Conclusion To recap, ovarian cysts are usually benign and occasionally have no symptoms at all. Occasionally, though, they can be painful, symptomatic and cancerous. If you’re experiencing any symptoms of ovarian cysts, please make an appointment with your healthcare provider as soon as possible.
Pregnancy: When is it Time to Go to the Hospital?

How to listen to labor symptoms and know when baby is really on the way. Whether this is your first baby or fourth, more than likely, you’ve got a bag packed for the hospital and sitting by the front door. (If you don’t, you should!) You’ve probably also got checklists on the fridge for family to get the mail, feed the pets and water the plants while you’re away. (Same here!) You’re as ready as you can be for baby to come. Being prepared is a great way to bring peace of mind to an otherwise stressful situation. But, when do you really know when it’s time to head to the hospital? Every woman’s journey is different and unique, but there are some signs of labor to look for as you’re waiting for baby’s arrival. Some are conveniently obvious, such as contractions and water breaking. But, other signs are more subtle. Signs of Labor Your water breaks. In only about 15 percent or less of women, water will break. If you’re fortunate to experience this obvious sign of labor, you know beyond a doubt that it’s time to head for the hospital. But, if you’re reading this blog, it’s likely because you may be experiencing more subtle signs. Keep reading to learn more. You’re having consistent contractions. These will become stronger and more frequent during labor onset. This is where all that knowledge from childbirth classes will kick in. Using a timer (there’s lots of apps for this in the App Store and on Android), time your contractions. If they are consistently happening every few minutes, it’s time to go to the hospital. Subtle Signs of Labor These signs are less obvious and can be more gradual. You’ll want to keep in touch with your doctor if you’re experiencing them. He or she can help you determine when to get in the car. The baby “drops.” This means your baby is getting into position for delivery, low within your pelvis. Your cervix dilates. During each visit as the due date draws near, your doctor checks whether your cervix is starting to dilate, or open, and/or efface, or thin out. You experience vaginal discharge and/or a change in color and consistency. You have diarrhea, loose-feeling joints, cramps, worsening back pain and fatigue. When to Call the Doctor During Late-Term Pregnancy If you’re not sure whether you’re experiencing any of these signs, it’s always best to call your provider, even if it’s after business hours. He or she will help you know if it’s time to hit the road for the hospital. Definitely give your doctor a call and head to the hospital in these situations: Your water breaks You notice bright-red discharge (blood) You develop a severe headache, blurred vision or sudden swelling. These are signs of preeclampsia. Our compassionate and experienced Grapevine and Fort Worth obgyns are here to help you have an informed, healthy pregnancy, labor and delivery. Contact us today for an appointment.
Your Path to Women’s Wellness

Three important steps to take on your path to women’s wellness Our Grapevine and Fort Worth obgyns urge you to take three significant steps on your path to women’s wellness. You can make it work, one step at a time. Your path to women’s wellness begins with these three critical actions Managing your health and attending your annual well-woman exam with our Grapevine and Fort Worth obgyns are vital steps on your path to women’s wellness. Here are some specific steps you can take to reach optimal health. Manage your overall wellness with a healthy diet and physical activity Part of your path to women’s wellness is getting to and maintaining a healthy weight. A normal body mass index (BMI) is between 18.5 and 24.9. The best way to achieve your weight goal is with a portion-controlled diet. This should consist of lean proteins, grains, vegetables, fruits and foods that provide calcium. Physical activity helps you build muscle, strong bones and a healthy heart. On your path to wellness, you should aim for 150 minutes of moderately intense activity such as brisk walking or bike rides. You should also add resistance training such as weight lifting or yoga. Pay attention to mental health issues such as stress and depression Your mental health is just as important as your physical health. Ignoring it can have adverse effects on your overall wellness. If you are suffering from stress, address it with your physician as part of your path to wellness. Stress can cause headaches, stomach problems, sleep issues and other physical symptoms. Depression is another undertreated and underreported problem, but it is a treatable medical issue. If you feel hopeless, sad or empty for more than two weeks, you may be suffering from depression. The right care can help you feel better. Schedule your annual well-woman exam with our Grapevine and Fort Worth obgyns A vital component of your path to women’s wellness is your annual well-woman exam. During this visit, we address your overall mental and physical health, schedule important health screenings and discuss other health issues. Annual appointments are our opportunity to get to know you better and care for your health. Contact us to schedule one.
Understanding Braxton Hicks Contractions

What to know about Braxton Hicks contractions Braxton Hicks contractions are often called false labor, but our Grapevine and Fort Worth obgyns understand that they can feel very real. Usually, women experience these pains during the third trimester, but sometimes they occur during the second trimester. They are a normal part of pregnancy, but they can be uncomfortable and cause concern because you may think you are in true labor. Three questions you may have about Braxton Hicks contractions The more you know, the less you will worry if and when you experience your first Braxton Hicks contractions. Here are three questions patients ask our Grapevine and Fort Worth obgyns about these contractions. What causes Braxton Hicks contractions? Physicians and researchers don’t know the exact cause, but one theory is that they occur because the uterus is expanding and the cervix is relaxing as the body prepares for true labor. Some people call it practice labor. Certain things can trigger these contractions such as a full bladder, dehydration, touching the belly and times when the mother and/or the baby are active. Women often notice these pains more often at the end of the day and also after sex. What do these false labor pains feel like? Braxton Hicks contractions are intermittent pains that cause the abdomen to tighten. They can last anywhere from a few seconds to one or two minutes at a time. How do I know if the contractions are Braxton Hicks or the beginning of labor? There are several differences between false labor and true labor. Braxton Hicks contractions usually don’t get stronger or closer together over time, but true labor contractions do. False labor pains can sometimes be alleviated or stopped by changing position, walking or resting. However, true labor pains cannot. Most false contractions only cause abdominal pain, but real labor pains can cause pelvic pressure and pain in the back, lower abdomen, and even the thighs. If you have any doubts about whether your contractions are Braxton Hicks or true labor, do not hesitate to call us. Our compassionate and experienced Grapevine and Fort Worth obgyns are here to help you have an informed, healthy pregnancy, labor and delivery. Contact us today for an appointment.
Three Tips for Selecting an Obgyn

Need help selecting an obgyn? Our Grapevine and Fort Worth obgyns have some tips to help you when you are selecting an obgyn. Your obgyn is an important part of your healthcare team. She not only performs your annual well woman exam and provides preventive healthcare, but she also helps you when you have problems and need gynecological services. When you decide to start or grow your family, your obgyn monitors your pregnancy and helps you have a healthy labor and delivery. Our Southlake and Fort Worth obgyns offer tips for selecting an obgyn Many women rely on referrals when selecting an obgyn, and that is a good place to start. However, our physicians have some other tips to help you pick an obgyn. Learn more about the physician’s background and credentials. Learn more about our obgyns’ education and experience. Our all-female Grapevine and Fort Worth obgyns provide compassionate healthcare for women of all ages. Many of our physicians have special areas of interest and expertise. If you are planning to become pregnant or are already pregnant, selecting an obgyn who is experienced in both routine and high-risk pregnancies is important. You will probably have a routine pregnancy, but in the event that you develop a high risk pregnancy, you want a physician who has experience caring for pregnancies with multiples, mothers with gestational diabetes and other issues that need to be carefully monitored during pregnancy. Our physicians have experience you can rely on to guide you through a healthy pregnancy, labor and delivery. Find a physician and staff who make you feel comfortable. Selecting an obgyn is a personal decision and one only you can make. You will need to develop a comfortable relationship with your physician so that you feel free to share personal information that your obgyn needs to care for you properly. You also should feel comfortable with the staff because you will interact with them before, during and after your appointments. From your first visit to Women’s Integrated Healthcare to every visit thereafter, our Southlake and Fort Worth obgyns and our staff strive to provide you with compassionate and experienced care. Selecting an obgyn doesn’t have to be intimidating. If you have any questions, contact us for an appointment.
Tips for Preparing for Gynecological Surgery

What you may not know about preparing for gynecological surgery Our Grapevine and Fort Worth obgyns believe that the more you know about preparing for gynecological surgery, the less nervous you will feel on the day of your procedure. You can help our surgeons by complying with all the instructions provided. Everything our physicians and staff advise you to do is for a reason, and following our directions makes the surgery and the recovery a smoother process. Five ways to prepare for gynecological surgery Some of our Grapevine and Fort Worth obgyns’ directions about preparing for gynecological surgery may surprise you and leave you wondering why you are being asked to do these particular things. Here are five critical steps to take before surgery and the reasons why our physicians ask you to follow these directions. Stop smoking cigarettes and marijuana. Smoking affects your heart and lungs, and so does anesthesia. When you stop smoking, your lungs begin to improve as early as 12 hours after you stop. Do not drink alcohol in the 24 hours before your surgery. Refraining from drinking prior to surgery is an important part of preparing for gynecological surgery. Alcohol affects how your body absorbs anesthesia and your blood’s ability to clot. Provide our obgyns with a complete list of every medication or supplement you take. Our Grapevine and Fort Worth obgyns need to know about every prescription and over-the-counter medication, as well as any vitamins, supplements or herbal remedies you take. Different ingredients can affect the medications our doctors need to administer during and after surgery. Remove nail polish and acrylic nails before surgery. This may seem like a small thing to do when preparing for gynecological surgery, but it’s essential. Surgeons and anesthesiologists need to see your natural nail bed to check for circulation problems. Do not shave for a certain amount of time before surgery. Ask our obgyns which areas of the body you should avoid shaving and for what period of time prior to surgery. Hair removal can leave nicks in the skin that increase your risk for an infected wound. Our compassionate staff and experienced Grapevine and Fort Worth obgyns make preparing for gynecological surgery as easy as possible. Our goal before and after surgery is a happy, healthy patient. Contact us for an appointment.
Do You Need Gynecological Surgery?
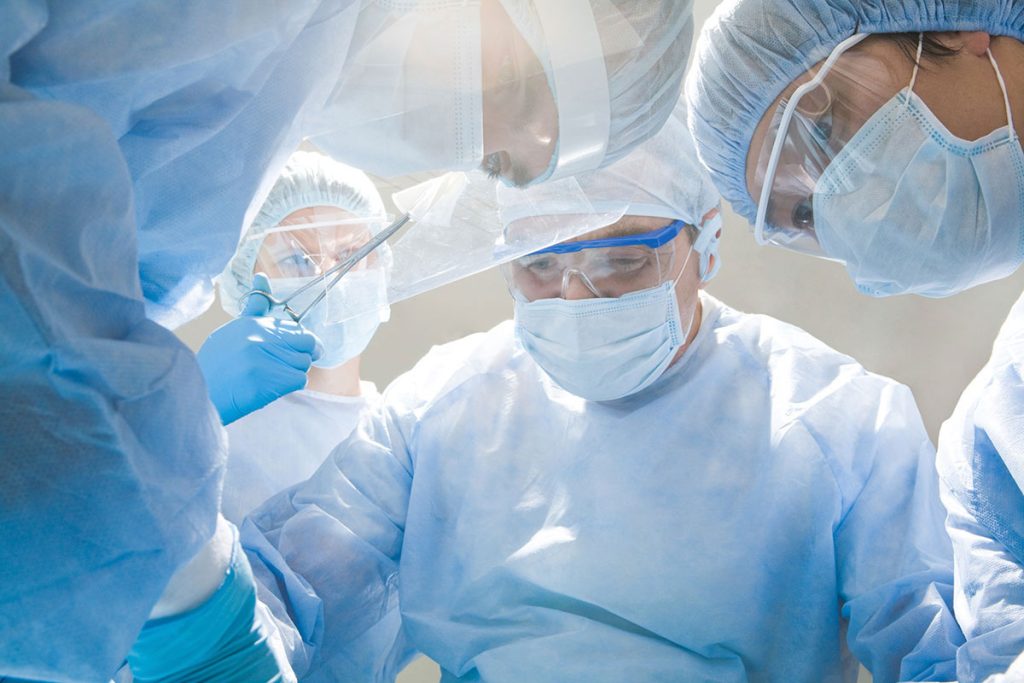
When do women need gynecological surgery? Our Grapevine and Fort Worth obgyns pursue several treatment options before considering gynecological surgery. However, in certain circumstances, surgery may be the best choice. Our experienced, highly trained surgeons perform the most-advanced minimally invasive surgical techniques, including da Vinci® robotic surgery. Leading-edge techniques help patients recover faster and with fewer complications than traditional, open surgery. When gynecological surgery is the best option After our Grapevine and Fort Worth obgyns have tried more-conservative treatment options, they discuss gynecological surgery with patients. Here are some common conditions that may require gynecological surgery to achieve a complete recovery. Endometriosis. Our physicians may perform a minimally invasive procedure called a laparoscopy to diagnose and treat endometriosis by removing endometrial implants. This surgery requires general anesthesia. In severe cases where the patient does not get pain relief from laparoscopic surgery, a hysterectomy may be necessary. Uterine fibroids. Fibroids cause a variety of symptoms, including menstrual problems, vaginal bleeding, cramps and infertility. Gynecological surgery helps women who have not responded to medication. Uterine fibroids may be removed during a myomectomy, a procedure where our surgeons remove the fibroids while leaving the uterus intact. Other procedures our obgyns may consider include endometrial ablation, hysteroscopy, uterine artery embolization or MRI-guided ultrasound surgery. In severe cases, hysterectomy may also be an option. Abnormal uterine bleeding. If medication doesn’t reduce heavy bleeding and long menstrual periods, gynecological surgery may be the optimal treatment. Our Grapevine and Fort Worth obgyns decide which type of gynecological surgery to perform based on whether the patient wants to have children, her age and her symptoms. Surgery ranges from endometrial ablation to uterine artery embolization. A hysterectomy may be necessary if other methods do not help with the bleeding. Leading-edge surgical techniques provide patients with better outcomes Our obgyns pursue advanced training and educational opportunities to give our patients the best care. Patients who are scheduled for surgery can rely on our Grapevine and Fort Worth obgyns’ skills and knowledge. Contact us for an appointment.
Honest Communication with Your Obgyn

What you should know about honest communication with your obgyn Our Grapevine and Fort Worth obgyns want you to know why honest communication with your obgyn is one of the most important things you can do for your health. Our physicians and staff are professionals who deal with women’s health issues every day. Everything you tell your obgyn is kept confidential, so you can be up front with us during your visits. Honest communication with your obgyn begins with these points Honest communication with your obgyn helps our physicians provide you with the best care. Your sexual history provides important information. Our Grapevine and Fort Worth obgyns need to know if you are sexually active. If you are, you may need to be tested for sexually transmitted infections (STIs) and be advised about safe sexual practices. It’s also important to tell us if you have pain or other symptoms during sex. Our Grapevine and Fort Worth obgyns need to know if you smoke, drink or use illegal drugs. Honest communication with your obgyn about habits like smoking, drinking or drugs may make you feel uncomfortable, but our obgyns are not here to judge you. Knowing about your habits helps us to assess your risk of certain illnesses. Our physicians also need to know about your lifestyle when you are thinking about becoming pregnant or are already pregnant so that we can advise you about protecting your baby. Don’t hesitate to tell us about embarrassing symptoms. You may think it’s awkward to mention things such as leaking urine or a diminished sex drive, but none of this makes our physicians uncomfortable. Honest communication with your obgyn means asking any and all questions. Avoiding scary symptoms will not make a problem go away. Finally, honest communication with your obgyn is crucial if you think you may have a serious problem. For example, if you are hesitant to mention a lump in your breast because you are afraid you have breast cancer, keep in mind that prompt diagnosis and treatment saves lives. When you visit our Grapevine and Fort Worth obgyns for your annual well-woman exam, gynecological services or obstetrics, talk to us openly and honestly so that we can provide you with the best care possible. Let’s talk. Contact us for an appointment.

